 
Currently, it would seem that subtotal colectomies/ERHs are largely unjustified in the elective setting as they are known to be associated with increased morbidity, slower recovery rates, and worse functional outcomes. The current literature seems to suggest that a more limited colon resection is indeed safe and can still provide adequate oncologic outcomes however, the few studies that do exist come from Europe and are based on single-center, retrospective studies. The preference for segmental resection of the splenic flexure is relatively low in several centers, while others strongly advocate for this colon-sparing option as it avoids unnecessary resection of the middle colic vessels and preserves colonic length. This has prompted some authors to evaluate the differences between these three surgical procedures and to also compare laparoscopic versus open approaches. Compared to a formal left hemicolectomy, a segmental resection also has a shorter operative time with equivalent post-operative morbidity. Splenic flexure resection for colon cancer is associated with an adequate lymph node harvest. However, on linear regression, segmental splenic flexure resection was associated with shorter operative time (estimate 20.29, 95%CI 12.61–27.97, p < 0.0001). After accounting for demographic, clinicopathologic, and operative factors, binomial logistic regression showed that type of procedure was not significantly associated with LN harvest (OR 0.80, 95%CI 0.54–1.17) or major morbidity (OR 1.17, 95%CI 0.36–3.81). 193 ± 84.1 min, p < 0.0001) and major morbidity was similar between the two surgical techniques (8.4% vs. Operative time was significantly shorter for segmental colectomy (213 ± 83.5 min vs. Inadequate nodal harvest (< 12 nodes) was infrequent and similar between the two procedures (7.4% vs. T- and N-stage did not differ between segmental and left hemicolectomy groups ( p = 0.703 and p = 0.429, respectively). 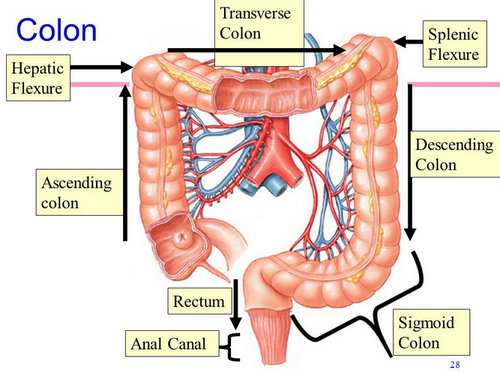
Of these, 83.6% had a segmental colectomy and 73% were performed by a minimally invasive approach. ResultsĪ total of 3,049 patients underwent colectomy for a splenic flexure cancer. 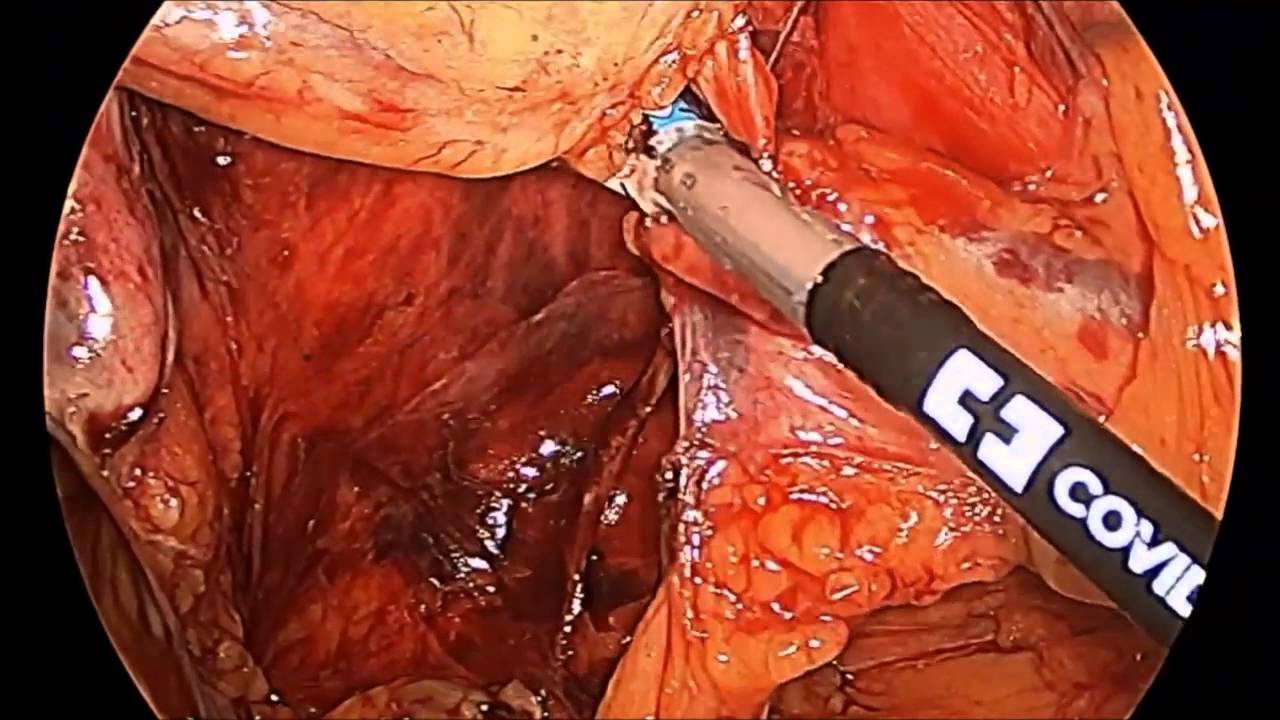
Factors independently associated with lymph node harvest, operative time, and post-operative morbidity were investigated by linear and binomial logistic regression models. Demographic, clinicopathologic, and post-operative outcomes were compared between groups. Patients were categorized based on type of surgical resection – left hemicolectomy with colorectal anastomosis or segmental colectomy with colocolonic anastomosis. Patients diagnosed with a splenic flexure cancer were identified from the 2012–2018 ACS-NSQIP colectomy-targeted database. The goal of this study was to compare lymph node harvest and post-operative morbidity between segmental resection and formal left hemicolectomy for splenic flexure colon cancers. A standard surgical approach to these cancers has not been defined. We consider this three-step method as being useful, and it might help the standardization of laparoscopic SFM.Fewer than 10% of colon cancers are found at the splenic flexure. No intraoperative complications were reported, including bleeding from the spleen and injury of the pancreas. Using this method, we performed laparoscopic SFM for 13 patients with colorectal cancer with no conversion to another approach or to open surgery. Third, the lateral attachment of the descending colon to the left abdominal wall is dissected cranially or caudally. The lesser sac is opened, and the attachment to the pancreas or spleen is cut using the inserted gauze as a landmark. Second, the transverse colon and transverse mesocolon are detached from the pancreas and spleen by means of an anterior approach. The appropriate plane for dissection can be recognized just beneath the inferior mesenteric vein, and the gauze should be placed in the dissected space. We propose a three-step method for laparoscopic SFM, aimed at providing a simplified and standardized method, which is presented in the video.įirst, the mesocolon of the transverse and descending colon is dissected from the retroperitoneal tissue using a medial approach. Although several approaches have been used for laparoscopic SFM,1 it is still considered complicated and troublesome because of the lack of a standardized technique. Splenic flexure mobilization (SFM) is sometimes required for secure and tension-free anastomosis during laparoscopic colorectal surgery. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
